Last updated 03.05.2026
Root canal infections: Symptoms and causes
Learn what causes root canal infection, common symptoms, treatment options and how early care protects your tooth.
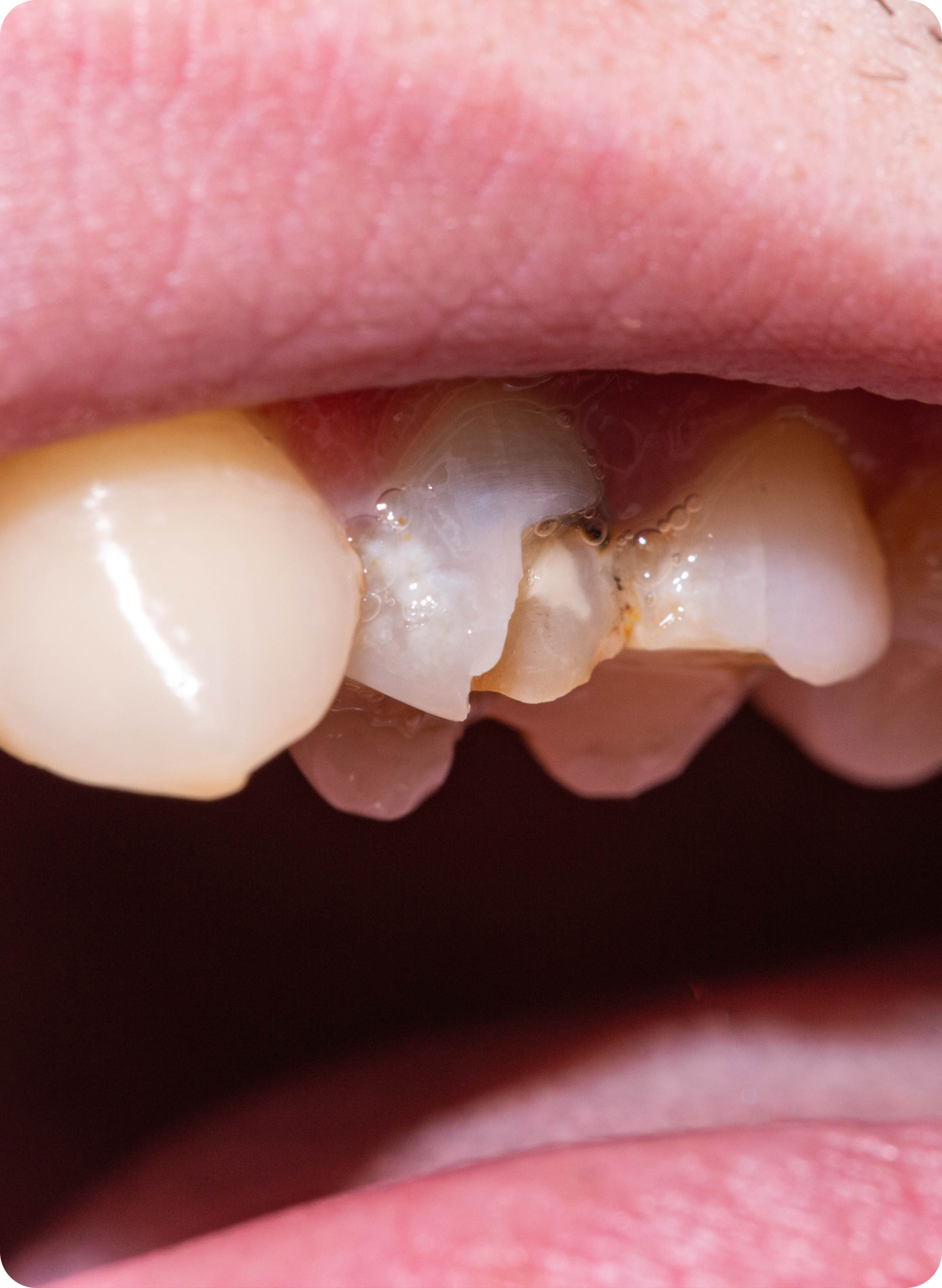
When it comes to restoring damaged or decayed teeth, a root canal may be required. However, there are some possibilities of infection after receiving a root canal. Understanding the symptoms and causes of root canal infections can help you seek timely care and maintain your oral health. Let's explore what you need to know about root canal infections.
Understanding root canals
Root canal treatments are designed to save teeth that have been severely damaged or will be damaged soon by the extent of decay or injury. The affected pulp is removed during the root canal procedure, and the tooth is sealed with tooth filling. However, in some cases, bacteria can persist or re-enter the tooth, leading to a root canal infection. While rare, these infections require prompt attention to prevent further complications.
The root canal procedure
The root canal procedure requires skill and precision, involving the use of specialized tools to clean out the infected pulp, shape the canal, and fill it with a biocompatible material. This aims to eliminate bacteria and prevent future infections. While the success rate is typically around 92.6%, according to the National Institute of Health, complications can arise due to the intricate anatomy of tooth roots and persistent bacteria. Understanding these factors can help you communicate effectively with your dentist and take necessary precautions for the best dental health outcome.
What is a root canal infection?
A root canal infection happens when bacteria penetrates the tooth's inner pulp, which contains nerves, blood vessels, and connective tissue. This can occur due to deep decay, repeated dental procedures, or tooth injuries. When left untreated, the infection can spread, causing pain and potentially leading to tooth loss.
Root canal infection symptoms
Root canal infections can manifest in various ways. Here are the most common symptoms to watch out for:
Persistent tooth pain
Severe, throbbing pain or toothaches that doesn't subside is often a sign of root canal infection. The pain may worsen when chewing or applying pressure to the affected tooth.
Sensitivity to temperature
Extreme sensitivity to hot or cold foods and beverages, especially if the sensation lingers after the stimulus is removed, could indicate an infected root canal.
Swollen gums
Inflammation around the affected tooth can cause the surrounding gums to become swollen, tender, or even develop a small, pimple-like bump.
Tooth discoloration
An infected tooth may darken or become discolored due to internal damage to the pulp.
Bad breath or taste
Persistent bad breath or an unpleasant taste in your mouth can be caused by the bacteria present in an infected root canal.
Loose tooth
In advanced cases, the infection can affect the surrounding bone, causing the tooth to feel loose.
What causes a root canal infection?
Deep decay
Untreated cavities can allow bacteria to reach the tooth's pulp.
Cracked, chipped tooth, or trauma
Damage or blow to the tooth's enamel can create an entry point for bacteria.
Repeated dental procedures
Multiple treatments on the same tooth can weaken its structure.
Gum disease
Advanced periodontal disease can allow bacteria to access the root canal.
Risk factors of root canal treatment infection
Several factors can increase your risk of developing a root canal infection:
Previous tooth injuries
Even minor cracks or chips can create vulnerabilities in your teeth.
Grinding or clenching
These habits can wear down tooth enamel, cause micro cracks, and trauma to the tooth over time.
Complex root anatomy
Teeth with intricate canal systems are more challenging to treat completely.
Immune system issues
Certain medical conditions or medications can make you more susceptible to infections.
Previous failed root canal
Teeth that have undergone multiple treatments may be more prone to complications.
Poor oral hygiene or delay in treatment
Neglecting or postponing proper dental care can introduce new bacteria to the treated area.
Benefits of early treatment
Treating an infection promptly offers several significant benefits. Pain relief is a primary advantage, as it alleviates the intense discomfort associated with infections. Early intervention can save your natural tooth from extraction, preserving it and preventing the infection from spreading to nearby teeth or the jawbone. This timely treatment not only promotes overall dental wellness but is also cost-effective, often being less expensive than addressing advanced complications.
✓ Pain relief
✓ Tooth preservation
✓ Prevention of spread
✓ Improved oral health
✓ Cost-effective
When to see a dentist for a failed root canal
Don't ignore potential signs of a root canal infection. Schedule an appointment with your dentist if you experience:
Persistent tooth pain
Prolonged sensitivity to temperature
Swelling or tenderness in your gums
Tooth discoloration
Persistent bad breath or taste
Any noticeable changes in your oral health
Treatment options for a failed root canal
Apicoectomy
When standard root canal treatments fall short, an apicoectomy can be a crucial procedure to save your tooth and prevent further complications. This specialized surgery targets the root tip (apex) of the tooth, addressing issues that conventional treatments may not resolve. The procedure involves making a small incision in the gum tissue to access the root tip, removing the infected tissue, and sealing the root end. While more invasive than a standard root canal, an apicoectomy is performed under local anesthesia to minimize discomfort.
Endodontic retreatment
When a root canal procedure doesn't fully resolve the issue or a new problem develops, endodontic retreatment offers a second chance to save your tooth. During retreatment, your dentist or endodontist will reopen the tooth, remove the original filling, and examine the internal structure. They'll clean and reshape the canals as needed, then place new filling material and seal the tooth. This process addresses issues missed in the initial treatment or that have developed since.
Tooth extraction
When all other treatment options have been exhausted, tooth extraction may become necessary as a last resort for managing severe root canal infections. Dentists and endodontists always prioritize saving your natural tooth whenever possible, as it's generally the best option for your oral health and function. However, in cases where the tooth is too severely damaged or infected to be saved through retreatment or apicoectomy, extraction might be the only viable option.
4 tips for preventing root canal infection
Maintain good oral hygiene
By brushing twice daily, flossing every day, and incorporating mouthwash into your routine, you can effectively remove plaque and bacteria, thereby lowering the risk of decay and infection.
Address issues promptly
If you’re experiencing issues with your root canal, it is best to seek professional help immediately to reduce any further complications or risk of infection.
Follow a healthy lifestyle
Eat soft foods, avoid chewing on the treated tooth if awaiting a crown, and refrain from smoking to ensure proper healing after treatment.
Follow dentist’s instructions
It is imperative that you follow your dentist’s instructions post-op, to prevent any damage to your tooth, post procedure.
Preventive care: Your path to a healthier smile
Remember, early detection and treatment of root canal infections significantly improve the chances of saving the tooth and preventing the spread of infection to other parts of your mouth or body. Don't hesitate to reach out to your dentist if you have any concerns or questions about your root canal treatment.
Root canal infection FAQs
How long do root canal procedures take?
A root canal treatment typically takes 1-2 appointments, each lasting about 60 minutes, depending on the complexity of the case.
Can a root canal infection spread?
Yes, if left untreated, a root canal infection can spread to surrounding teeth, gums, and even to other parts of the body. This is why prompt treatment is crucial.
How can I provide root canal infections?
Maintain good oral hygiene, visit your dentist regularly, avoid excessive sugar consumption, and address any tooth injuries or decay promptly to reduce your risk of root canal infections.
What happens if I don’t treat a root canal infection?
Untreated root canal infections can lead to severe pain, abscess formation, bone loss, and eventually, tooth loss. In rare cases, the infection can spread to other parts of the body, causing serious health complications.
Are there alternatives to root canal treatment?
The primary alternative to a root canal is tooth extraction. However, preserving your natural tooth through root canal treatment is often the preferred option when possible.
Can I go back to work after a root canal procedure?
Most patients can return to their normal activities the day after the procedure. However, it's best to avoid strenuous physical activity for a few days following treatment.
How successful are root canal treatments?
Root canal treatments have a high success rate, with many treated teeth lasting a lifetime with proper care and maintenance.
What should I do if I suspect a root canal infection?
If you're experiencing symptoms of a root canal infection, contact your dentist immediately for an evaluation. Early diagnosis and treatment can significantly improve outcomes and potentially save your tooth.